In the evolving landscape of diabetes management, continuous glucose monitoring (CGM) devices have emerged as game-changers for individuals managing diabetes. These innovative tools allow users to keep track of their glucose levels in real time, significantly improving their ability to manage their condition. At National Diabetic Supply, we believe understanding how to maximize the effectiveness of your CGM device is crucial for achieving better health outcomes.

Understanding Your CGM Device
Before you start using a CGM device, it’s essential to thoroughly understand how it works. These devices typically consist of a small wearable sensor placed just under the skin that continuously measures glucose levels in interstitial fluid. Familiarize yourself with the device’s various components, including the sensor, transmitter, and mobile app or receiver that displays glucose data. This is vital to ensure accurate readings and effective use.

Calibrating Your Device
Many CGM devices require calibration to ensure accuracy. This process usually involves taking fingerstick blood glucose readings using a glucose meter and inputting these values into the CGM device. Follow the manufacturer’s instructions carefully for calibration frequency and methods. Regularly calibrating your device can improve the reliability of glucose readings and provide you with the data needed to make informed decisions about insulin dosages and dietary choices.
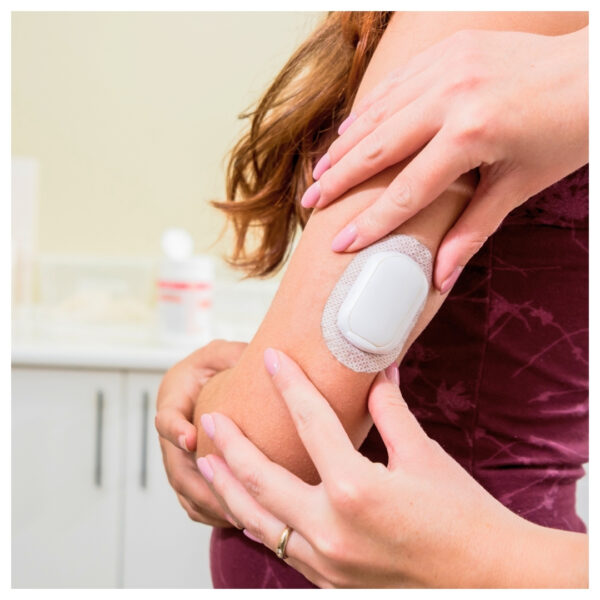
Site Selection and Sensor Placement
Proper site selection for your CGM sensor is critical for reliable measurements. Choose areas with adequate fat tissue, such as the abdomen or the back of the arm, to reduce discomfort and the risk of sensor failure. Make sure the skin is clean and free of oils before applying the sensor to ensure a strong hold. Following the manufacturer’s placement guidelines can enhance the sensor’s longevity and effectiveness.
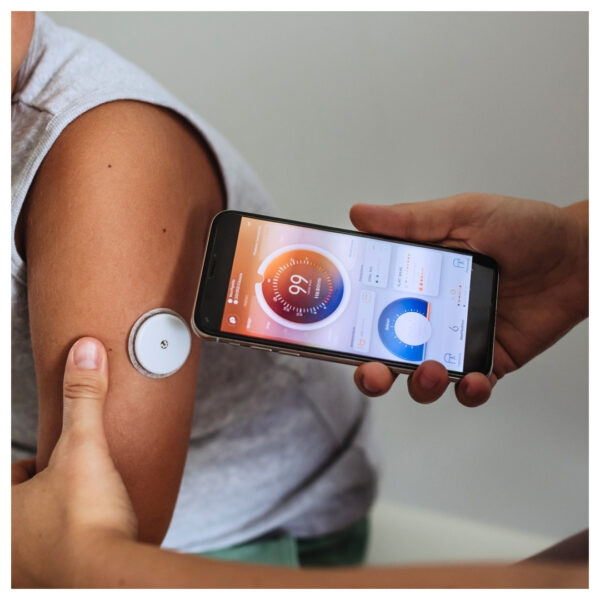
Monitoring Trends and Patterns
One of the greatest benefits of using a CGM device is its ability to display glucose trends over time. Regularly reviewing these trends can help you identify patterns related to food intake, physical activity, and stress levels. By understanding how your body responds to different factors, you can make proactive adjustments to your diabetes management plan.
Responding to Alerts and Notifications
Modern wearable glucose monitors often come equipped with alert systems that notify you of high or low glucose levels. These alerts can be customized based on your personal preferences. It’s vital to pay attention to these notifications and respond promptly to avoid severe hypoglycemic or hyperglycemic episodes. Ignoring alerts can lead to complications, so stay engaged with your device and trust the data it provides.

Engaging With Your Healthcare Team
Maintaining open communication with your healthcare team is essential while using a CGM device. Share your glucose data with your doctor or diabetes educator, who can help you interpret the information and make informed adjustments to your management plan. Your healthcare provider can also assist you in establishing personalized goals based on CGM data, ensuring you are on the right path to successful diabetes management.
Using a CGM device effectively requires understanding your device, calibrating it properly, selecting the right sensor sites, monitoring trends, and engaging with alerts. At National Diabetic Supply, we offer a range of diabetic supplies to support your journey. Explore our selection to optimize your diabetes management!
Shop Now
